
By John P. Porcari, Ph.D., Katelyn Falck-Wiese, M.S., Samantha Suckow-Stenger, M.S., Jillian Turek, M.S., Anna Wargowsky, M.S., Maria L. Cress, M.S., Scott T. Doberstein, M.S., Chelsea J. Hahn, M.S., Abigail L. Ryskey, M.S. and Carl Foster, Ph.D., with Daniel J. Green
Traditionally, exercise programs have been developed using range-based protocols. For example, commonly accepted fitness-industry guidelines are typically based on exercisers working at a percentage of their heart-rate reserve (HRR), oxygen consumption reserve (VO2R), maximal heart rate (MHR) or maximal oxygen consumption (VO2max). Unfortunately, the ranges provided are often so broad that they provide very little real guidance to health coaches and exercise professionals.
Additionally, to compound the problem, you would have to conduct a maximal exercise test with each client in order to program exercise using HR or VO2 guidelines, which is impossible in most settings due to both cost and time. Because of this, for some time researchers have tried to develop an equation that can accurately predict maximal heart rate in lieu of doing the maximal exercise test. While they have improved somewhat since the early days of “220 – Age,” these equations are still pretty unreliable. For instance, if a trainer is using %HRR to program exercise for clients, even if two individuals have the same MHR (whether measured via testing or estimated using an equation), and therefore the same target heart rate during exercise, the metabolic overload may be very different depending on whether the target heart rate is above or below the individual’s ventilatory threshold.
Is there a better way to individualize a client’s exercise intensity from the outset so that you’re not wasting valuable time in the beginning of a program when most clients are so prone to dropout?
ACE enlisted the help of John Porcari, Ph.D., and his team of researchers in the Department of Exercise and Sport Science at the University of Wisconsin–La Crosse to investigate whether the Talk Test provides a suitable alternative to range-based programming and provokes training responses that are comparable to traditional guidelines.
The Talk Test and the First Ventilatory Threshold
Ventilatory threshold testing, including the Talk Test, is based on what happens to ventilation during an incremental exercise test. As exercise intensity increases, ventilation increases in a somewhat linear manner. The deflection points seen in Figure 1 are associated with metabolic changes within the body. The first notable point is called the “crossover” point and represents a level of intensity where the body can no longer supply its energy needs aerobically, so it needs to begin supplementing that with anaerobic metabolism. A byproduct of anaerobic metabolism is lactic acid, which begins to accumulate in the blood. That lactic acid is buffered by bicarbonate, which results in an excess production of carbon dioxide. This excess carbon dioxide stimulates ventilation further, resulting in the first nonlinear increase in ventilation. This first deflection point is termed the first ventilatory threshold (VT1).
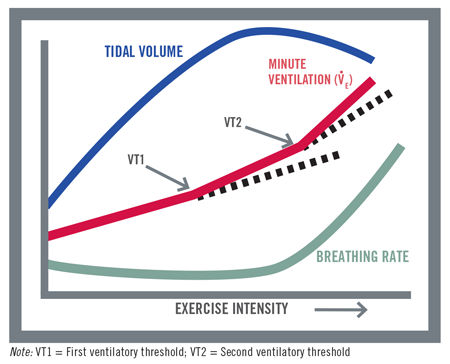
The objective of the Talk Test is to identify the point at which talking first becomes uncomfortable-to-challenging, but not impossible. This point coincides with VT1. Stated simply, if the client can perform the exercise and talk comfortably in sentences that are more than a few words in length, he or she is likely below his or her VT1. Once a client starts to have difficulty, he or she is at or above VT1. The full protocol for the Talk Test can be found in each of the ACE manuals. Note that the Talk Test can also be used to determine the second ventilatory threshold (VT2), but that was not the focus of this study.
The Study
The researchers recruited 44 university-aged individuals, 17 male and 27 female, all of whom were sedentary. The participants were randomly divided into two groups that were matched in terms of age, height, weight and VO2max, which was determined prior to the beginning of the study.
Both groups completed a 10-week progressive exercise program consisting of three 40-minute sessions per week using a cycle ergometer (30 minutes of exercise, plus a 5-minute warm-up and a 5-minute cool-down). A consistent pedaling rate of 60 rotations per minute (rpm) was used, with adjustments in power output (PO) accomplished by increasing the resistance on the bike’s flywheel.
The HRR Group exercised at 40 to 59% HRR (moderate exercise) for weeks 1 through 4. For weeks 5 through 8, they exercised at 50 to 69% HRR (the high end of moderate exercise), and then progressed to 60 to 79% HRR (the low end of the vigorous exercise range) for weeks 9 and 10.
The TT (Talk Test) Group exercised at the highest PO that still allowed for comfortable speech, meaning that they consistently exercised at or just below their individualized VT1.
For both groups, intensity was assessed every five minutes during each workout. For the HRR Group, the intensity was adjusted as needed to stay within the target range. Those in the TT Group recited the first 101 words of the Rainbow Passage and were asked whether they could “speak comfortably.” If they answer was a clear “yes,” then PO was increased by approximately 30 Watts (W). If the answer was either “no” or a tentative “yes,” PO was decreased by approximately 30 W. Heart rate and RPE were also recorded in this group to document the intensity of training, but this data was not used to regulate training intensity.
The Results
The participants’ acute responses to the training are presented in Figure 2. Training intensity, whether expressed in terms of PO (W/kg), %HRR or ratings of perceived exertion (RPE), was significantly higher in the TT Group during the first eight weeks of training as compared to the HRR Group. As the intensity progressed in the HRR Group as described above, the differences between the two groups gradually declined.
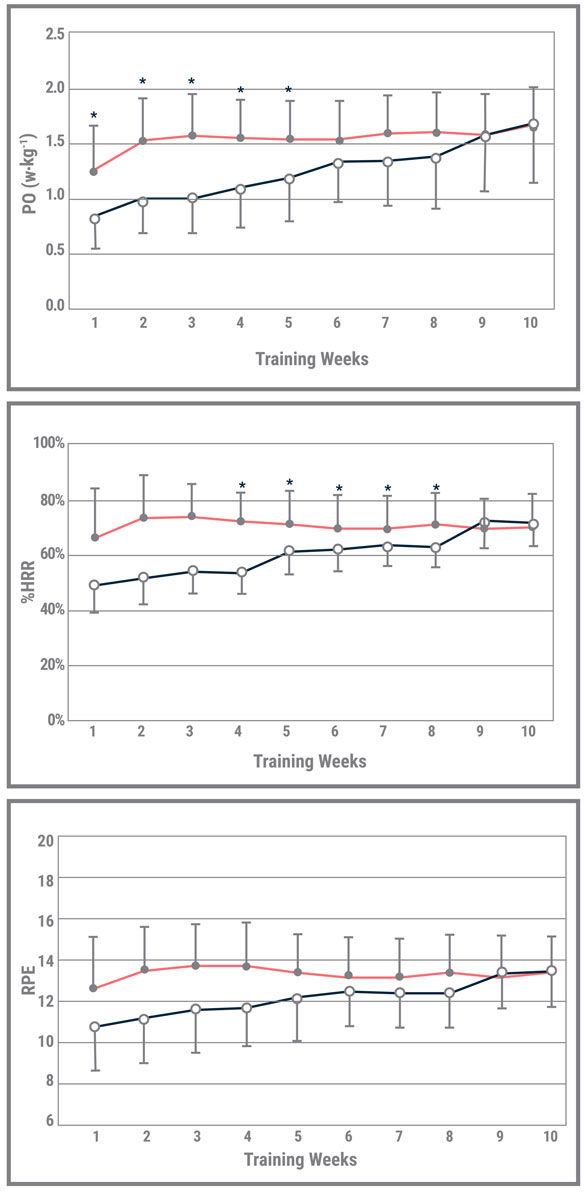
Figure 2
Acute training responses in the Talk Test (TT) (closed symbols) and Heart Rate Reserve (HRR) (open symbols) groups across the 10 weeks of training. Data represent mean and standard deviation. Significant differences between the groups are represented by an asterisk (*). There were no significant interaction terms within the data analysis.
According to Dr. Porcari, these findings clearly illustrate the advantages of the Talk Test for exercise programming, as those in the HRR Group were not working nearly as hard as those in the TT Group for the first eight weeks of the 10-week study. Think of that in a real-world scenario in which you’re working with a new client. If it takes you up to two months of trial and error to find the intensity at which the client will derive the most benefit from the program, you are risking boring—and potentially losing—the client during that period when he or she is most vulnerable to dropout. In contrast, those in the TT Group were working at a higher, but still comfortable, intensity from the outset.
By the end of the 10 weeks, all 44 participants were exercising at similar levels, as can be seen in Figure 2. “This proves that you don’t need an expensive maximal exercise test to identify an appropriate training intensity,” according to Dr. Porcari. “The Talk Test will get you and your clients to the same place.”
Overall, the training intensity in both groups fell within the recommended training window for all measures. As expected, there was a progression of PO in both groups, which reflects the fact that a higher PO was required to satisfy the monitoring criteria for training intensity. In other words, the participants worked harder over the course of the 10 weeks, denoting an increase in physical fitness.
When looking at the improvements in performance found in each group, peak PO, VO2max, PO and VO2 at VT1, and HR at VT1 improved similarly in each group, while maximal HR remained unchanged. What this means is that exercise capacity, no matter how and when it was measured, improved to the same extent regardless of whether the intensity of training was guided by the Talk Test or %HRR (Figure 3).
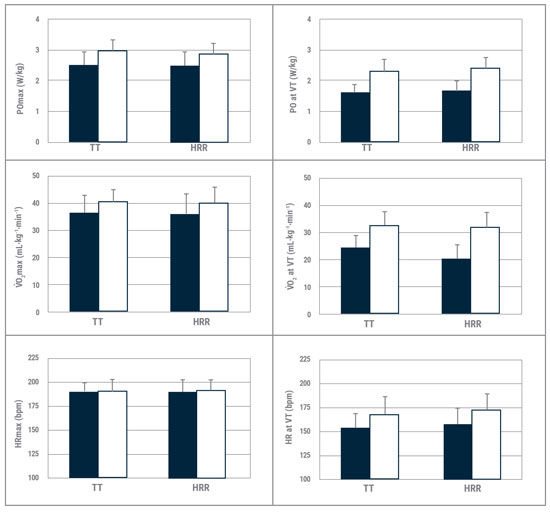
Figure 3
Changes in maximal responses and responses at the ventilatory threshold (VT) consequent to the training in the Talk Test and Heart Rate Reserve groups. The solid bars represent pretesting values and the open bars represent posttesting values. Data represent mean and standard deviation.
Exercise Enjoyment
Once each week for the duration of the study, the researchers assessed participants’ enjoyment of the workout five minutes before, at the midpoint, and five minutes after the training session. What they found was that members of both groups reported a steady decline in how much they enjoyed the workouts (Figure 3). Part of this may be due to the fact that all 30 workouts performed were exactly the same and were of a moderate intensity, which is typically not the most exciting type of exercise. That said, Dr. Porcari highlights the importance of variety in a training program, in terms of intensity, modality, setting and a host of other variables. Keeping your clients interested and happy with a program is a major key to long-term success and adherence.
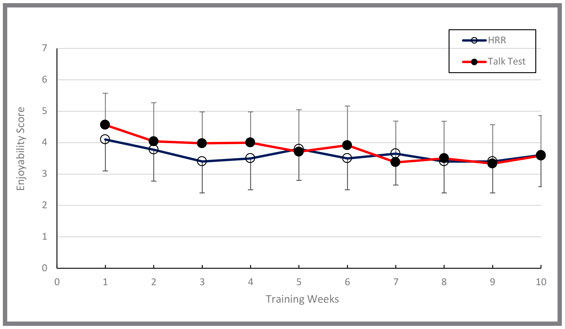
Figure 4
Changes in exercise enjoyability during exercise in the Talk Test (closed symbols) and Heart Rate Reserve (open symbols) groups across the 10 weeks of training. Data represent mean and standard deviation.
The Talk Test and the ACE Integrated Fitness Training® (ACE IFT®) Model
The ACE IFT Model is featured in the ACE Personal Trainer Manual and summarized in other ACE texts and continuing education offerings. The Cardiorespiratory Training component of the ACE IFT Model was built upon the utilization of the Talk Test, which is first introduced in Phase 1: Aerobic-base Training. In that phase, clients are encouraged to exercise at an intensity that allows them to talk comfortably, meaning that they are below their VT1.
During Phase 2: Aerobic-efficiency Training, aerobic intervals are introduced at a level that is at or just above VT1. The goal of these intervals is to improve aerobic endurance by raising the intensity of exercise performed at VT1, and to improve the client’s ability to utilize fat as a fuel source.
During Phase 3: Anaerobic-endurance Training and Phase 4: Anaerobic-power Training, higher-intensity intervals are introduced that load the cardiorespiratory system enough to develop anaerobic endurance. The key is to balance training time spent below VT1 (70 to 80%), between VT1 and VT2 (<10%), and at or above VT2 (10 to 20%). In Phase 4, those intervals performed at or above VT2 will be at a higher intensity, of a shorter duration, and with a longer recovery period than those performed in Phase 3.
Summary
This study provides evidence that supports the efficacy of Talk Test–based exercise programming and, therefore, of the ACE IFT Model. By eliminating the need for cost-prohibitive and time-consuming assessments, these findings enable health and exercise professionals to offer truly individualized exercise programming to their clients, which will improve adherence and drive better results. Stated simply, using the Talk Test allows you to train clients without having to perform maximal exercise testing or rely on exercise heart rates to guide intensity. Instead, you can have clients exercise just below the intensity at which they lose the ability to talk comfortably—this is VT1. The use of the Talk Test dramatically simplifies what has always been one of the most complex elements of exercise programming—identifying the right intensity to effectively and safely drive results.
“These findings truly revolutionize the concept of exercise programming,” explains Dr. Porcari, “as they demonstrate that exercise professionals can provide individualized intensity monitoring and exercise programming using a free and easy assessment that can be performed in almost any setting.”
Note: This study was first published in the peer-reviewed journal Kinesiology.
References
American College of Sports Medicine (2018). ACSM’s Guidelines for Exercise Testing and Prescription (10th ed.). Philadelphia: Wolters Kluwer.
American Council on Exercise (2014). ACE Personal Trainer Manual (5th ed.). San Diego: American Council on Exercise.





 by
by 







