
By Lance C. Dalleck, PhD, Karrie M. Butler, MSc, and Christina A. Buchanan, PhD, with Daniel J. Green
College students are particularly prone to what has been called the “active couch potato” syndrome. That is, they live active lifestyles, often meeting the recommended guideline of 150 minutes of moderate-intensity cardiorespiratory exercise per week, but also spend a lot of time doing sedentary activities, such as sitting for long periods as they attend classes, study, and watch TV or play video games. Unfortunately, individuals who are sedentary but physically active are at a higher risk of cardiometabolic disease than those who are equally active but spend less time being sedentary (Yates et al., 2011).
In other words, meeting the physical activity guidelines alone is not enough to overcome the negative effects of high amounts of daily sedentary behavior.
Cardiovascular disease (CVD) is widespread in the United States but is largely preventable through lifestyle change. College students are typically perceived to be relatively healthy and as having a low risk for CVD, dyslipidemia and obesity (the last two of which are risk factors, along with physical inactivity, for CVD). However, this may not necessarily be the case. Because they are often more active than other adults and see doctors less often, college students may not be aware of the presence of these risk factors.
For example, Dalleck and Kjelland (2010) found that 6.8% of college students had metabolic syndrome, a cluster of conditions that increases a person’s risk for developing heart disease, type 2 diabetes and stroke. In addition, 13.0% had two risk factors for metabolic syndrome and 42.5% exhibited one risk factor; the risk factors for metabolic syndrome are elevated waist circumference, elevated triglycerides, reduced high-density lipoprotein cholesterol, increased blood pressure and elevated fasting blood glucose.
Fortunately, important health benefits can be derived from reducing sedentary time, entirely separate from those gained through physical activity. ACE asked Lance C. Dalleck, PhD, and his team of researchers in the High Altitude Exercise Physiology Program at Western Colorado University to examine the effects of standing in the college classroom setting on cardiometabolic risk factors among college students.
The Study
The research team recruited 21 students to participate in this study (Table 1). All participants had at least two classes in a particular building on campus (where researchers placed the standing desks), and none were pregnant or had an injury or medical condition that would prevent them from standing for an extended period of time.
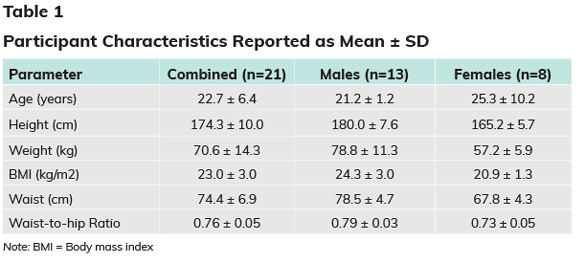
In addition to the values presented in Table 1, researchers obtained resting blood pressure, fasting lipids and fasting blood glucose as baseline measures before the study began.
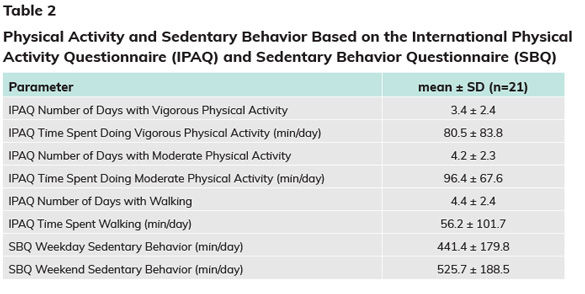
Participants filled out two surveys regarding physical activity and sedentary behavior: the International Physical Activity Questionnaire (IPAQ) and the Sedentary Behavior Questionnaire (SBQ). The participants, on average, met commonly accepted physical-activity recommendations (American College of Sports Medicine, 2018). However, despite the higher than average physical-activity levels, the participants’ sedentary behavior time is considered excessive (Table 2).
The participants were randomly divided into two groups. Group 1 stood at a standing desk during a class session on at least two occasions, totaling a minimum of five hours, per week. Group 2 sat during those same class sessions. After a one-week wash-out period during which all participants were required to sit, the two groups switched roles, with group 2 standing and group 1 sitting.
Importantly, the participants were instructed to avoid leaning on their desks or other stationary objects while using the standing desks to avoid contamination of the results. They were also not encouraged to stand outside of their requirements for this study and they were asked each week if they attended their classes, stood in those classes and whether they left class early. Total standing hours were recorded for each participant.
Each week throughout the study, with the exception of the wash-out week, the researchers again measured resting blood pressure, fasting lipids and fasting blood glucose. On one occasion during the study, a metabolic cart was used to measure gas exchange data between standing and sitting for each participant to establish the metabolic demands of these activities (Figure 1).
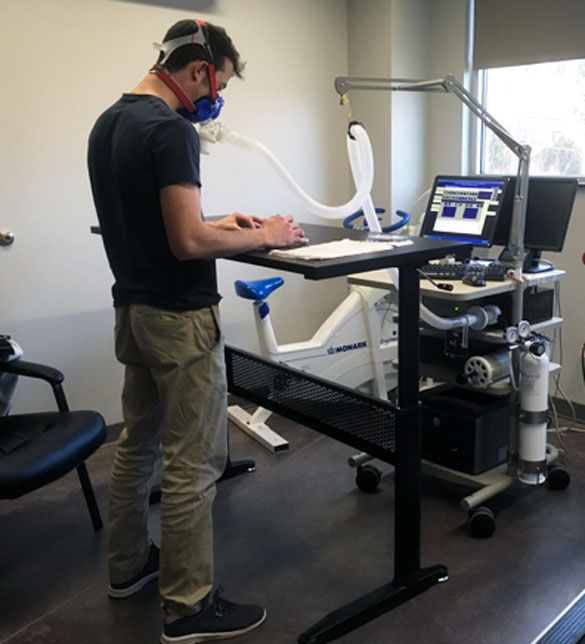
Figure 1. A study participant attached to the metabolic analyzer during the measurement of standing METs.
The Results
The measurements for the cardiometabolic risk factors during three weeks of sitting and three weeks of standing are presented in Table 3. Statistically significant differences were seen in all risk factors between the sitting and standing time blocks. The metabolic equivalents of sitting and standing (as measured using the metabolic cart) were also significantly different.
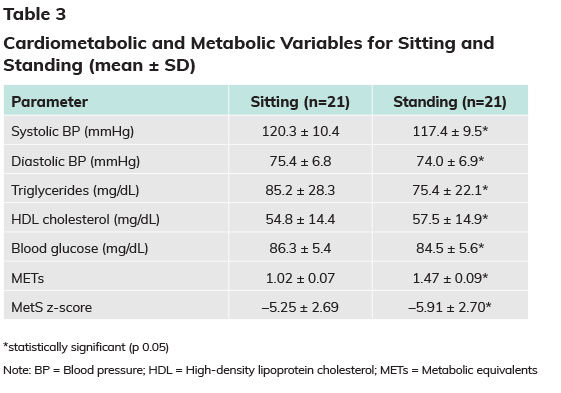
Traditionally, researchers looking into training responsiveness have used maximal oxygen uptake (VO2max) exclusively to quantify improvements in cardiorespiratory fitness, which provides a very narrow view. The MetS z-score (see Table 3) is a means of measuring training responsiveness that combines a number of cardiometabolic risk factor values into a single continuous score, including blood pressure, circumference measures, blood glucose, high-density lipoprotein and triglycerides (Malin et al., 2013). The primary benefits for inclusion of a continuous MetS z-score are twofold: (1) it acknowledges that there is a continuum to cardiometabolic risk within each individual and (2) it provides a more sensitive tool for assessing individualized training responsiveness following an exercise intervention.
“By broadening the assessment of training responsiveness using the MetS z-score, researchers are better able to capture the true benefits of an exercise program,” explains Dr. Dalleck.
While there was considerable variability among the participants in this study, there was a 100% incidence of a favorable change in the MetS z-score response to standing versus sitting (Figure 2).
In other words, every student who took part in this study experienced a positive change in all risk factors as a result of simply replacing five hours of sedentary time per week with standing.
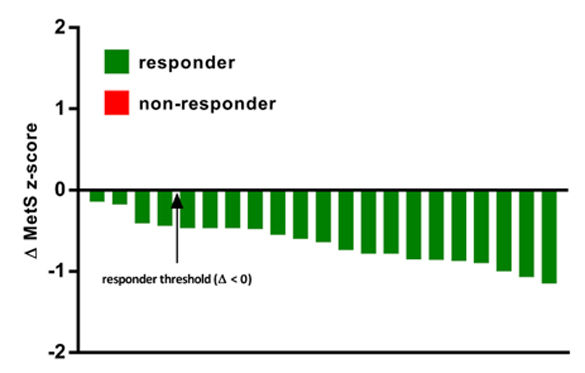
Figure 2. Inter-individual variability in change in MetS z-score responses to standing when compared to sitting
"Every student who took part in this study experienced a positive change in all risk factors as a result of simply replacing five hours of sedentary time per week with standing."
The Bottom Line
The research team identified four key takeaways from this study:
- Use of a standing desk in the classroom was found to significantly improve cardiometabolic health throughout a short three-week timespan.
- Results indicate that the study participants satisfied recommendations for physical activity; however, the participants also engaged in substantial periods of sedentary behavior, potentially negating the positive benefits of regular physical activity.
- The intervention was well-tolerated and therefore may be a promising modality to improve the cardiometabolic profile of people who engage in large amounts of sedentary behavior.
- Increasing standing time in the classroom, and therefore lessening weekly sedentary behavior, could be a potential wide-scale, effective strategy for the prevention of chronic disease.
This is all great news, as replacing five hours of sitting per week with five hours of standing is a very reasonable protocol to combat the considerable ill effects of a sedentary lifestyle. “While the positive changes are elicited fairly quickly,” says Dr. Dalleck, “it’s important to acknowledge that these effects are short-lasting, which means consistency is key.”
Fortunately, students seem to prefer the standing option. In another study, it was found that 95% of university-based students preferred the option to stand when it was offered (Benzo et al., 2016).
This brings us to an important point: Subtly adjusting the classroom environment by replacing some sitting desks with standing desks may be a sufficient impetus to alter students’ behavior enough to help improve cardiometabolic health in the university setting. This is an example of something called “choice architecture,” which involves altering the built environment to reduce the need to use willpower to drive positive lifestyle choices—think of keeping a bowl of fruit on the kitchen table instead of a candy jar.
The results of this study represent a call to action to not only health and exercise professionals, but also school and university administrators, as simply offering the option to stand during class may result in meaningful improvements to the health and well-being of students of all ages. As the research team says, “This group [of university-age students] was reasonably healthy and still saw positive change…. What would the cardiometabolic profiles of college students look like had they been standing in class since kindergarten? The current trend in primary education is to provide different ‘workstation’ options for children, where they can choose to sit or stand. As children progress, however, through secondary school and then into college, the norm is to keep people in their seats. Therefore, by the time one gets into the workplace, these habits are well formed and the road to poor health has been set in motion. The good news is that, based on the modest yet significant changes seen in this study with three weeks of standing in the classroom, regardless of when sitting behavior changes during the lifespan, cardiometabolic risk factors may be reduced, reversed or even prevented altogether.”
References
American College of Sports Medicine (2018). ACSM’s Guidelines for Exercise Testing and Prescription (10th ed.). Philadelphia: Wolters Kluwer.
Benzo, R.M. et al. (2016). Learning to stand: The acceptability and feasibility of introducing standing desks into college classrooms. International Journal of Environmental Research and Public Health, 13, 8. pii: E823. doi: 10.3390/ijerph13080823.
Dalleck, L.C. & Kjelland, E.M. (2012). The prevalence of metabolic syndrome and metabolic risk factors in college-aged students. American Journal of Health Promotion, 27, 1, 37–42.
Malin, S.K. et al. (2013). Metformin modifies the exercise training effects on risk factors for cardiovascular disease in impaired glucose tolerant adults. Obesity, 21, 93–100.
Yates, T. et al. (2011). Stand up for your health: Is it time to rethink the physical activity paradigm? Diabetes Research and Clinical Practice, 93, 292–294.





 by
by 








