
How many of your clients first came to you after being told by their doctors that they needed to lose some weight? With the ever-increasing number of people who are struggling with overweight or obesity, doctors are undoubtedly issuing this directive more and more often. But what does a patient do with this information? It’s not as though he or she can simply go home and “lose some weight.” Presumably, the intention behind the doctor’s recommendation is a desire to improve the patient’s health, but is equating weight loss with health really in the patient’s best interest—and is it even accurate?

Health at Every Size
Harriet Brown highlights the Health at Every Size (HAES) movement as a tool to redirect the conversation so that it focuses on health instead of weight. HAES challenges the significance of promoting weight loss and dieting behavior and argues for a shift in focus to weight-neutral outcomes. The HAES approach is associated with statistically and clinically relevant improvements in physiological measures (e.g., blood pressure and blood lipids), health behaviors (e.g., eating and activity habits and dietary quality) and psychosocial outcomes (e.g., self-esteem and body image). What would it look like if you focused on supporting clients’ improved health behaviors, such as eating more lean protein and fruits and vegetables and/or being active most days of the week, instead of on weight loss?
Consider the following guidelines when discussing HAES with clients:
- Continue to help set healthy behavioral goals that are specific, measurable, attainable, relevant and time-bound, such as adding an additional high-intensity workout to the week.
- Long-term goals should focus on health, not weight.
- Interventions should have a holistic focus and consider the physical, emotional, social, occupational, intellectual, spiritual and ecological aspects of health.
- Programs should focus on promoting self-esteem, self-efficacy, body satisfaction and body-size diversity.
- Interventions should focus on modifiable behaviors to improve health and not weight.
- Weight is not a behavior.
“There is tremendous value is separating health from weight,” says Harriet Brown, associate professor of magazine journalism with a focus on health and science journalism at Syracuse University and author of Body of Truth: How Science, History and Culture Drive Our Obsession With Weight—and What We Can Do About It. “Not everyone can lose weight and keep it off,” Brown says, “but everyone can perform behaviors that improve their health.”
Behavior Vs. Outcome
Losing weight is not a behavior, but rather one outcome among many when a person changes his or her lifestyle. In other words, weight loss is not a driver of change but a consequence of change. Weight loss is often misunderstood by clients as being the first step in improving health. The misconception lies in the belief that weight loss leads to improvements in blood pressure and glucose levels, for example, when the truth is overweight and obesity are items on the list of interrelated elements of morbidity that can be addressed through increased physical activity and better nutrition.
In the conclusion of her book, Brown provides a list of what she personally needs to do to “feel healthy and creative” and “joyful, physically and emotionally.” This list, of course, will be different for everyone, but it should include things like eating more fruits and vegetables, getting adequate sleep and performing physical activities on a daily basis that bring you joy, whether that is dancing, hiking or walking on the treadmill while you binge-watch a favorite show. The point is to figure out what makes you happy, or to help each individual client identify what makes him or her happy, and then develop a plan to make that happen. Weight loss is a likely outcome of this lifestyle change, but it doesn’t have to be the primary motivator.
The Relationship Between Weight and Health
Focusing on weight—and modern culture certainly has an obsession with the topic—typically brings negativity into something that should be all about positivity. If a client comes to see you only because she wants to lose weight, her motivation is always going to be teetering on the brink depending on the number on her bathroom scale. In addition, much of her self-talk will likely be weight-focused and overwhelmingly negative and critical. If you can instead encourage her to think about her new lifestyle as something that brings her improved health and even joy, then her motivation—and her self-defined successes and failures—will be less reliant on the singular outcome of weight loss.
Equating thinness with health is an especially risky proposition for certain segments of the population. As described by Brown in Body of Trust, the toxic culture around thinness, dieting and physical appearance can lead to destructive obsessive behaviors, including life-threatening eating disorders.
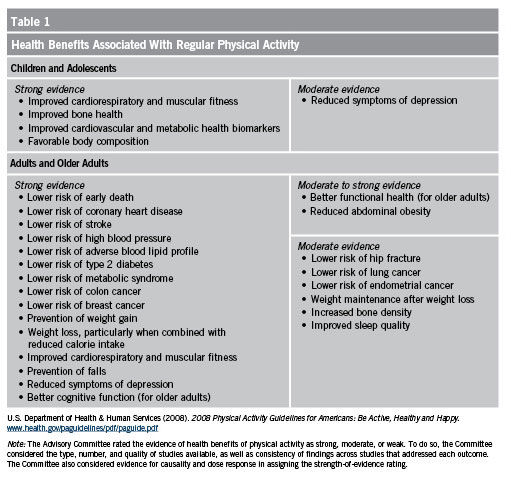
It is important that clients understand that increased levels of physical activity and improved nutritional intake are the driving forces behind not only weight loss, but also the countless other benefits of physical activity—and these can be achieved with or without the concomitant weight loss (Table 1). Note that this article focuses on physical activity because that is solidly the within the purview of health and fitness professionals. That said, though changes in diet are important in one’s overall health and essential to long-term weight maintenance, the benefits listed in Table 1 can be seen with increases in physical activity alone.
“Evidence has shown that an overweight, yet active person will have a better overall health profile than a thin, inactive person,” explains Cedric X. Bryant, Ph.D., ACE’s Chief Science Officer. That overall health status is defined by objective measurements including VO2max, blood lipid profile and glycemic control rather than the way a person looks. “That said,” Dr. Bryant continues, “We also know that with weight loss you will see more improvement in cholesterol measures, particularly triglycerides, better glycemic control, less insulin resistance and improvements in blood pressure.”
Stated simply, while health improvements occur with physical activity alone, weight loss will optimize those effects. Long-term sustainability of health is best achieved, says Dr. Bryant, with a balanced approach that includes healthy eating, appropriate doses of exercise and living a more active lifestyle that includes moving more throughout the day.
The Cost of Carrying Extra Weight
Just as it is important for your clients to understand that improved health does not necessarily require substantial weight loss, it is essential for them to know that there are real and meaningful risks associated with carrying extra pounds.
“Carrying extra weight exposes joints structures to higher levels of risk, explains Dr. Bryant. “Remember, the ground reaction forces and impact forces experienced during physical activity are directly proportional to the exerciser’s body weight.” Therefore, a jogger, for example, who is overweight despite a high physical-activity level is going to struggle to stay injury-free over the long term because of the wear and tear on his body.
In addition, there are some well-recognized associations between obesity and risk factors for cardiovascular disease (National Heart, Lung and Blood Institute, 1998). Of particular importance is the relationship between body fat that is localized in the abdominal area—called visceral adiposity—and systemic inflammation. Evidence suggests that cardiovascular disease, type 2 diabetes and the metabolic syndrome are all linked to the proinflammatory state associated with abdominal obesity (Lee and Pratley, 2007; Wisse, 2004; Fasshauer and Paschke, 2003). Obese individuals are much more prone to these cardiometabolic diseases than the general population.
Fortunately, increased physical activity and/or fitness may attenuate the systemic inflammation associated with visceral adiposity (Mora et al., 2006; Panagiotakos et al., 2004; Church et al., 2002). Evidence also suggests that being physically active can reduce the risk of cardiovascular or all-cause mortality associated with being overweight or obese (Farrell et al., 2002; Lee, Blair, and Jackson, 1999). Additionally, regular exercise (especially moderate-to-vigorous activity) has been shown to reduce the risk of developing type 2 diabetes (Morrato et al., 2007; Sullivan et al., 2005).
Conclusion
Good health and the attainment and maintenance of a “normal” weight are inextricably linked. As demonstrated in this article, weight loss potentiates the effects of physical activity and allows an individual to work toward optimum health. Body composition—the makeup of the body in relation to proportions of lean body mass and body fat—is an important element of health and physical fitness and should not be overlooked.
That said, many clients would benefit from downplaying the measurable long-term effects of physical activity and weight loss, and instead focus on the relatively rapid improvements in well-being and quality of life. When working with clients who have had life-long struggles with the scale, you can help them have positive experiences with exercise, focus on those physical activities they most enjoy and, yes, even teach them to find personal joy and fulfillment through movement. This can be particularly valuable early in your relationship with a new client or during those inevitable stretches when clients experience a lapse in motivation. In those moments, tell them to set aside the numbers and have some fun. Once you’re up and moving, the benefits, including weight loss, take care of themselves.
References
Brown, H. (2015). Body of Truth: How Science, History, and Culture Drive Our Obsession with Weight—and What We Can Do about It. Philadelphia: Da Capo Lifelong.
Church, T.S. et al. (2002). Associations between cardiorespiratory fitness and C-reactive protein in men. Arteriosclerosis, Thrombosis, & Vascular Biology, 22, 1869–1876.
Farrell, S.W. et al. (2002). The relation of body mass index, cardiorespiratory fitness, and all-cause mortality in women. Obesity Research, 10, 417–423.
Fasshauer, M. & Paschke, R. (2003). Regulation of adipocytokines and insulin resistance. Diabetologia, 46, 1594–1603.
Lee, C.D., Blair, S.N., & Jackson, A.S. (1999). Cardiorespiratory fitness, body composition, and all-cause and cardiovascular disease mortality in men. American Journal of Clinical Nutrition, 69, 373–380.
Lee, Y.H. & Pratley, R.E. (2007). Abdominal obesity and cardiovascular disease risk: The emerging role of the adipocyte. Journal of Cardiopulmonary Rehabilitation, 27, 2–10.
Mora, S. et al. (2006). Association of physical activity and body mass index with novel and traditional cardiovascular biomarkers in women. Journal of the American Medical Association, 295, 1412–1419.
Morrato, E.H. et al. (2007) Physical activity in U.S. adults with diabetes and at risk for developing diabetes. Diabetes Care, 30, 203–209.
National Heart, Lung and Blood Institute (1998). Obesity Education Initiative Expert Panel. Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults: The Evidence Report. Bethesda, Md.: National Institutes of Health. NIH publication No. 98-4083.
Panagiotakos, D.B. et al. (2004). The associations between leisure-time physical activity and inflammatory and coagulation markers related to cardiovascular disease: The ATTICA study.
Preventive Medicine, 40, 432–437.
Sullivan, P.W. et al. (2005). Obesity, inactivity, and the prevalence of diabetes and diabetes-related cardiovascular comorbidities in the U.S., 2000–2002. Diabetes Care, 28, 1599–1603.
U.S. Department of Health & Human Services (2008). 2008 Physical Activity Guidelines for Americans: Be Active, Healthy and Happy.www.health.gov/paguidelines/pdf/paguide.pdf
Wisse, B.E. (2004). The inflammatory syndrome: The role of adipose tissue cytokines in metabolic disorders linked to obesity. Journal of the American Society of Nephrology, 15, 2792–2800.





 by
by 





