As a health and fitness professional, there is a wide range of clients that you can choose to focus on and include as a part of your business. It is possible, however, that you may be overlooking a significant segment of the population that desperately needs the guidance of a qualified health and fitness professional—those who experience chronic pain. Here's how you can help.
Defining Chronic Pain
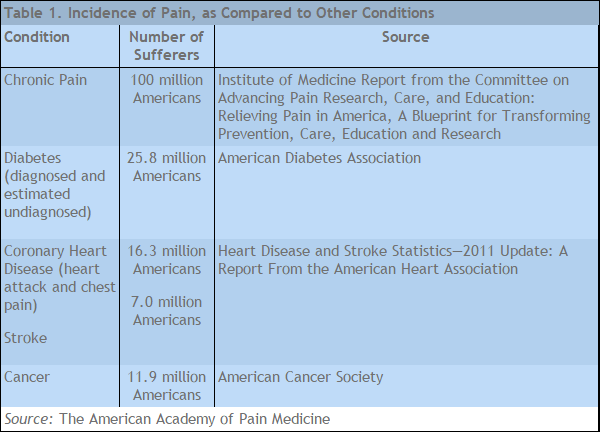
According to the American Academy of Pain Medicine, more than 100 million Americans are affected by chronic pain (Table 1), which is more than diabetes, heart disease and cancer combined. Chronic pain can be defined as persistent pain that may plague a person for weeks, months or even years, and the effects can be debilitating.
Among Americans who suffer from chronic pain, the most prevalent complaint is low-back pain (27 percent). Other common complaints include headaches, neck pain and facial pain. Equally staggering is the amount of money that is lost due to the effect of chronic pain on the U.S. workforce. The American Academy of Pain Medicine compared data released in 2010 from the Institute of Medicine with data from a 2003 study published in the Journal of the American Medical Association. In 2003, U.S. businesses experienced a $61.2 billion loss due to decreased productivity caused by chronic pain Stewart et al., 2003). In 2010, this number jumped to a whopping $297.4 billion (American Academy of Pain Medicine, 2014).
So we know that there are millions of people suffering from chronic pain, but what can you, the health and fitness professional, do to expand your business and help this group of clientele so in need of your services?
Step #1 – Create a referral network.
According to the American Academy of Pain Medicine (2014), 63 percent of adults who experience chronic pain have sought help from their family physician. Creating a referral program with a local doctor is a great way to increase business while helping those who likely need your services.
Start with your own doctor and ask him or her for advice on how your efforts would be best received. It is important for the medical community to see you as an asset rather than a threat to their business or to the patient/client. Make sure you have information about how you can help their patients and be sure to let the physician know that referrals work in two directions (everybody wins). Referrals for chronic pain from a physician to a fitness professional should not overstep the bounds of a physical-therapy referral, but can be a part of the long-term overall health-improvement and pain-management plan.
Creating a referral network with physical therapy offices is also an important part of the cycle. Once a client is released from physical therapy, he or she is likely to go back to his or her previous behaviors that caused the chronic pain. This is where you can be particularly helpful in helping the individual achieve long-term behavior change. In many cases, people find at-home rehabilitation programs to be challenging to do on their own, because they have to rely on their own initiative and motivation to complete the recommended exercises. For those clients who may not possess the appropriate level of intrinsic motivation to accomplish the tasks asked by their physical therapist, having a relationship with these clients and their therapists can help everyone achieve their goals and remain pain-free.
Creating a positive word-of-mouth referral network is the best way to attract this type of clientele, explains Justin Price, ACE Certified Personal Trainer and creator of the Biomechanics Method: Exercise Solutions for Chronic Pain. “[When] this type of referral source comes from a third party that the client trusts, the client in chronic pain will come to you with a lot more trust in your services. This initial trust will work wonders in helping build the necessary rapport and the close communication that is needed to help design the highly individualized programs that are required to help people overcome chronic pain.”
Step #2 – Understand why your client is in pain.
There are countless reasons why someone may suffer from chronic pain. Perhaps they were in a traumatic car accident years ago, or they were born with a genetic musculoskeletal issue. Most of the individuals who suffer from chronic pain, however, may have never experienced an acute incident and were never diagnosed with a genetic issue or disease.
According to the 2013 State of American Well-being report released by Gallup-Healthways, obesity rates are still at their highest point and are contributing to physical pain felt on a regular basis. When an individual reaches out to a personal trainer for weight loss, he or she recognizes the need to lose weight. However, the person may not realize that his or her current body-fat percentage may also be contributing to chronic pain.
Anthony Carey has traveled the globe working with clients and educating fitness professionals about helping those who suffer from chronic pain. “Every new client’s first appointment begins with an intake that is very extensive,” explains Carey, an ACE Certified Personal Trainer and owner of Function First in San Diego, Calif. “We spend a significant amount of time educating them on the pain process and how it relates to movement and exercise.”
It is important to remain within the scope of practice when working with clients; therefore, performing a comprehensive health-history questionnaire and an exercise history and attitude questionnaire are helpful first steps in learning about why a client may be in pain. From your clients’ answers, you may be able to delve deeper into why they experience chronic pain. If they answered “Yes” to “Do you have, or have you had in the past: difficulty with physical exercise,” be sure to ask follow-up questions such as, “What type of difficulty have you had with exercise in the past?” or “Can you describe how you feel when you do physical activity?”
Asking questions that require more than a simple “yes” or “no” response allows the client to open up and helps create a level of trust between the two of you. Be sure to actually listen to your client’s responses and take his or her past experiences into account when planning the program.
Step #3 – Understand your scope of practice and the biomechanics involved.
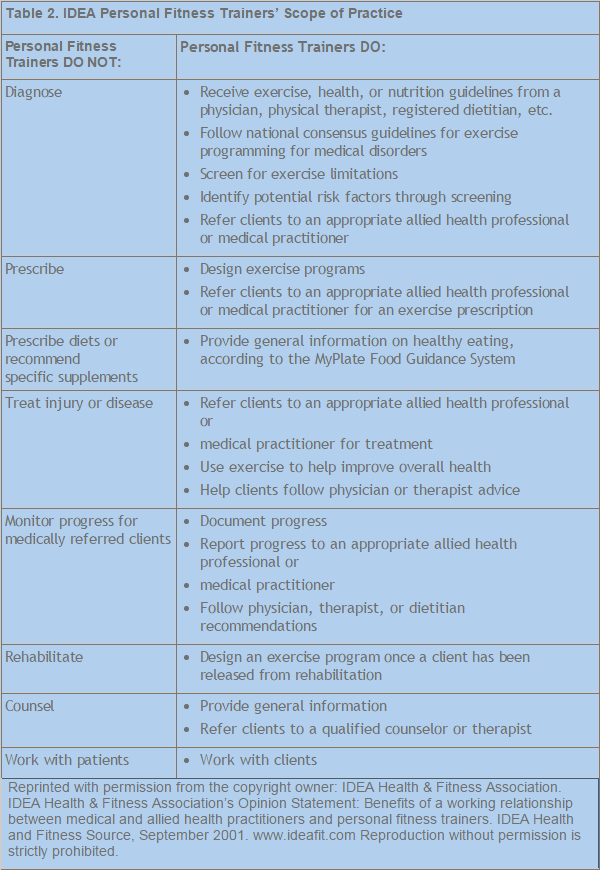
Within the fitness industry, there is a very thin line between assessments/screenings and diagnosing why a certain musculoskeletal issue exists. Remember, as a fitness professional, it is outside your scope of practice to diagnose an injury or prescribe treatment such as medications or supplements. However, it is fully within your scope of practice as a fitness professional to perform exercise screenings to understand any limitations the client may have (Table 2).
“Because a lot of professionals have assured clients that they can help and yet haven’t been able to, many people will have a lot of fear and anxiety about their condition and will likely be very wary of your ability to help them overcome their chronic pain,” cautions Price. “Therefore, it is extremely important that you begin very slowly with this type of clientele and ask for their continual feedback about what works and what doesn’t so that they guide the progression of their program.”
For many people, chronic pain resides around large joints or areas in the body that compensate when the next large joint in the chain is injured or does not have enough mobility or stability to appropriately control or provide movement. Understanding how all of the major areas along the kinetic chain work is essential to understanding the body as well as where pain may manifest itself. Figure 1 shows the major areas of body and whether those areas are meant to provide stability (resist movement) or mobility (allow for movement).
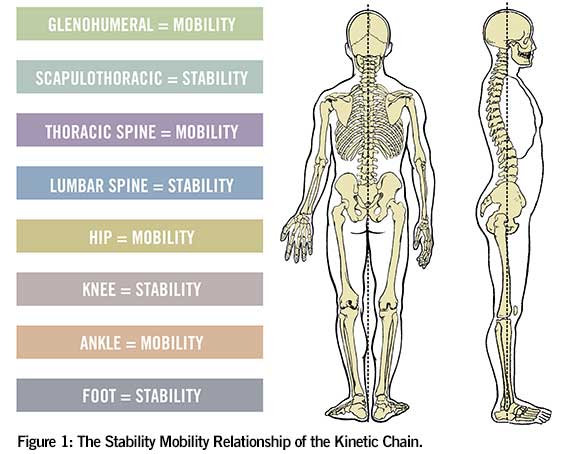
When performing static postural assessments or movement screens, it is essential to keep this image in mind. For example, during a bend-and-lift screen, you may notice that a client has limited range of motion in the ankles and is unable to dorsiflex his or her feet. Because the ankle is supposed to supply the body with mobility for walking, running and traversing uneven surfaces, the likely place a client may experience pain up the kinetic chain is the knee, hip or low back.
In short, it is important for you to be aware of the pain that clients are feeling and why they might be experiencing pain (without diagnosing anything), and be able to provide guidance as to how the client can improve his or her current pain level.
“We have to understand the many contributing factors to chronic pain,” says Carey. “The characteristics of acute pain and chronic pain are significantly different on many levels. If we want to provide services to this population, we can’t expect to simply apply a more conservative exercise program to them. Everything from the environment we provide our services in to the descriptive language we use dramatically impacts their experience.”
References
American Academy of Pain Medicine (2014). The Cost of Pain to Business and Society Due to Ineffective Pain Care.
Institute of Medicine of the National Academies (2011). Relieving Pain in America: A Blueprint for Transforming Prevention, Care, Education, and Research. The National Academies Press, Washington, D.C.
Stewart, W.F. et al. (2003). Lost productive time and cost due to common pain conditions in the U.S. workforce. Journal of the American Medical Association, 290, 18, 2443−2454.





 by
by 





