
By Amanda Vogel, M.A.
Imagine this frightening scenario: A client, Susan, who you’ve been training for a few months comes in for her usual workout at one o’clock in the afternoon on Monday. She begins jogging on the treadmill, but within 10 minutes is complaining of itchy skin, trouble breathing, stomach pains and dizziness. She looks flushed, and her skin appears to have broken out in hives. Alarmed, you get her to stop exercising immediately and call 911.
What happened? Susan is fairly fit and was only going at a moderate pace, so you know overexertion wasn’t the problem. And she wasn’t sick either; in fact, she’d arrived for the session in good spirits, having just come from a lunch date with friends where she’d enjoyed a tuna-with-celery sandwich.
Turns out, Susan experienced a rare, total-body allergic reaction called exercise-induced anaphylaxis (EIA), which is brought on by exercise or exercise plus additional factors, such as certain food(s) ingested around the time of exercise (for Susan, it was the chopped-up celery in her sandwich).
While exercise-induced anaphylaxis is not at all common—some experts say it affects about one in a thousand people—symptoms can occur among those who have not previously shown any signs.
“It has been estimated that EIA may represent 5 percent to 15 percent of all cases of anaphylaxis,” says Brian Smart, M.D., an allergist and immunologist at the DuPage Medical Group Asthma and Allergy Center in Glen Ellyn, Ill. Although EIA is uncommon, fitness professionals should be aware of this potentially serious condition and its associated variables.
What Is Exercise-induced Anaphylaxis?
In defining exercise-induced anaphylaxis, it’s important to clarify that it isn’t actually a true allergy to exercise, which, of course, sounds like the world’s greatest excuse for staying sedentary.
“The term ‘allergy to exercise’ is misleading and evokes a mental image of someone sitting on a couch eating chips, saying, ‘I am allergic to exercise.’ The term exercise-induced anaphylaxis is more accurate and less sensational,” says Smart.
“People who exercise and get anaphylaxis are not allergic to exercise,” agrees Timothy J. Craig, D.O., professor of medicine and pediatrics at Penn State University’s College of Medicine in Hershey, Pa. “Exercise, for some reason, causes them to have anaphylaxis.”
But why? As mentioned, combining exercise with certain foods—or any food, for some people—can result in anaphylaxis. (These subsets of EIA are discussed in greater detail below.)
“With regard to exercise-induced anaphylaxis unrelated to co-ingestion of foods, there are notions that exercise in the pollen season, high heat, extreme cold, high humidity or more extreme exercise may be a factor,” says Scott H. Sicherer, M.D., a professor of pediatrics at Jaffe Food Allergy Institute, Mount Sinai School of Medicine in New York. “However, these factors have not been confirmed. Also, there are descriptions of people having exercise-induced anaphylaxis from mild exercise (such as raking leaves).”
With EIA, the word “anaphylaxis” can best be explained as a spectrum of exercise-induced allergic symptoms, all of which should be taken seriously. “Some people just get flushing and hives when they exercise. Other people might get lightheaded and/or nauseated. Some people get wheezing,” says Craig. “You can get the full constellation or you can have a component. But probably, most commonly, we see flushing or hives.”
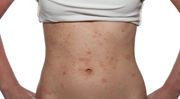
Cholinergic Urticaria
Another condition that may affect exercisers is cholinergic urticaria, which some experts see as either a milder presentation of exercise-induced anaphylaxis (EIA) or a separate entity altogether. It is likely more common than exercise-induced anaphylaxis. “There are people who get hives from sweating or being overheated or sometimes cooled,” explains Sichere. “This could occur during exercise, but also with exposures like hot showers or swimming, depending on the exact condition.” People with this condition can often avoid symptoms by controlling exercise environment and temperature.
General symptoms to look out for include:
- skin swelling and rashes (such as hives, mosquito-bite-like rashes)
- itching and flushing
- asthma symptoms/trouble breathing
- choking
- gut symptoms (abdominal pain, nausea, vomiting)
- poor blood circulation (resulting in dizziness, confusion, paleness, loss of consciousness)
“If the episode becomes full-blown, it may include loss of consciousness, cardiovascular collapse and death,” says Smart. “Life-threatening episodes and fatalities have been reported, but are quite uncommon with this condition.”
Craig estimates that of all his patients with EIA, only about five in the last 10 years have actually lost consciousness from the allergic episode. Regardless, anaphylaxis should be treated seriously and a client with this condition should stop exercise at the first sign of symptoms. Trainers must be careful to heed their clients’ concerns—do not tell a client who presents with symptoms that the feelings are “all in their head.”
While symptoms can occur at any time during or after exercise, they are most likely to start in the first 30 minutes of activity. “People of any age, race or gender can get EIA, but it is seen most often in people in their 20s and 30s,” says Smart.
Food-associated Exercise-induced Anaphylaxis
While it’s not always clear why a person experiences EIA, there are two subsets of EIA that make detecting the trigger a little easier. These subsets involve food consumed close to the time of exercise. One subset is related to specific foods ingested; the other involves any food at all. These occurrences are known as food-associated exercise-induced anaphylaxis (FAEIA) or food-dependent exercise-induced anaphylaxis (FDEIA).
“Even though the particular food may be tolerated without symptoms, and exercise may be tolerated without symptoms, the combination of eating the food(s) and exercising results in anaphylaxis,” explains Sicherer.
Specific Foods
One subset of EIA involves one or more specific foods causing an allergic reaction when consumed close to the time of exercise. “This subset of people don’t have symptoms if they eat the food only. If they exercise only, they don’t have symptoms. But when they eat the food and go on to exercise, they have symptoms. You need the combination of the food and exercise together in order to get symptoms,” explains Craig.
Smart says this subset is estimated to be about one-third to one-half of all EIA cases. Many foods can bring on an allergic reaction, but some of the most common trigger foods are wheat, celery, tomato, seafood (especially shellfish) and peanuts. “Aspirin and other NSAIDs, like ibuprofen, can worsen symptoms,” says Smart. It’s theorized that these substances might change the body’s ability to filter allergens.
Any Food
The other food-related subset involves any food plus exercise, leading to anaphylaxis. “So it’s not a specific food,” says Craig. “And that’s more difficult because you don’t have a positive [allergy] skin-test that you can hang a hat on.”
For this group of people, the best and safest approach is to avoid eating for four or more hours before exercise and at least an hour afterward. Since this approach can be tricky for some people, exercising first thing in the morning before breakfast might be the best solution.
Why Does FAEIA Happen?
Experts are still figuring out why some foods, when associated with exercise, might lead to EIA. “We do not know why the combination results in a reaction, but there are theories,” says Sicherer. “The theories include that exercise causes a change in the way some foods (for example, wheat) are digested, making them more allergenic; that the exercise causes blood flow to be shifted in a way that carries food proteins to more allergy cells in the body; or that the gut absorbs food differently during exercise. It may also be that the exercise alters the body’s allergy susceptibility due to changes in the blood salts and acids during exercise, making allergy cells activate more easily to any triggers, perhaps some that are not a problem when not exercising.”
Craig offers this explanation about why exercise might cause such a reaction with food: “It seems that exercise, which causes dilation of vessels, is somehow able to activate mass cells to release histamine. And that’s probably what’s occurring—the neurologic mechanism or the phenomenon that causes vessels to dilate or mass cells to release the histamine, and the overflow of histamine is causing all those symptoms.”
Avoidance and Treatment of EIA Symptoms
Fitness professionals who are aware of EIA and FAEIA can help a client with this condition maintain an active lifestyle as safely and effectively as possible. It’s a good idea to always err on the side of sensitivity and caution rather than disagree or dismiss a client who reports pain or discomfort consistent with an anaphylactic reaction.
Resources
American Academy of Allergy, Asthma & Immunology (AAAAI)
The Food Allergy & Anaphylaxis Network (FAAN)
Encourage the client to work with a qualified allergist (see sidebar for resources), who can order tests to help the client determine contributing factors. This ensures a proper diagnosis and treatment plan. “There are a variety of medical conditions that can mimic exercise-related anaphylaxis, so it is important to discuss the exact symptoms with an allergist,” says Sicherer. “Do not self-diagnose or make assumptions. Very often, there is some other explanation for allergy symptoms during exercise and these must be addressed to reduce symptoms and improve health and safety. There are no simple reliable tests for the condition. There appears to be a degree of unpredictability, where a reaction may or may not occur under what appear to be similar conditions.”
“The good news is,” adds Sicherer, “that the problem often reduces or resolves with time. People with this diagnosis can usually continue to exercise with various precautions in place.”
In addition to identifying if one or more foods might be the trigger, clients should consider other factors. For example, exercise intensity may play a role, but not every time. “Any degree of exercise can cause symptoms, but more intense exercise is more likely to do so,” says Smart. “However, these episodes are inconsistent and an intense workout one day may not cause symptoms, while a recovery session another day could cause symptoms.”
Exercise environment may also be a consideration. “For susceptible people, exercise in very hot, very cold or very humid weather should be avoided,” says Smart. “This is probably for reasons of increased stress and, consequently, increased gut permeability/altered blood flow, etc. For people who also have seasonal allergy, outdoor exercise in pollen seasons can also trigger episodes, presumably because of increased circulating mediators of allergy.”
As far as treatment goes, Sicherer warns that simply taking an antihistamine before exercise is not considered a useful treatment (although it might reduce the rate of reactions for some people). He recommends these precautions: “The person with this illness must always carry emergency medications and an auto-injector of epinephrine, wear medical identification jewelry, carry written emergency instructions and carry a cell phone,” says Sicherer. It’s also wise to exercise with a buddy or trainer who is aware of the condition and how to recognize and respond to anaphylaxis (this includes halting exercise and calling emergency medical services).
What about avoiding exercise altogether? It’s not necessary. “I strongly encourage regular exercise for virtually all my patients,” says Smart. “Most patients with EIA/FDEIA, with caution and a good treatment plan, can still exercise,” says Smart.
Craig agrees. “I never tell people not to exercise,” he says. “Exercise is such an important thing for people’s health. I try to work around it.”
One Woman’s Struggle With Extreme Itchiness During Outdoor Exercise
Paige, 43, is an English teacher in Escondido, Calif. Growing up, she played team sports and says she’s always been active. She works out at the gym three to four times a week and does yoga once a week. For her, exercising can be quite uncomfortable due to the extreme itchiness brought on by exercising in certain environments. Here is Paige’s story.

“I experience really strong anxiety in connection with the itching. My heart rate increases. So, it’s not just a local reaction. It’s a different sensation than an itch from a bug bite. Sometimes, it’s so extreme that I scratch the area excessively, which results in red welts and scratch marks.
“I played soccer in middle school and high school, and I remember dealing with the itching, especially during morning games. The problem does not seem to be as severe as it once was, but that might be because I’ve altered my exercise regime. The symptoms rarely happen in the gym, where I do most of my workouts these days.
“The best way I’ve found to ease the situation is to relax my breathing (I’ve learned to do that through yoga and meditation). That usually means ending the workout, at least temporarily.”
NOTE: The information presented in this article is not intended as a diagnosis or recommendation of treatment. A client who presents any allergic symptoms during exercise should immediately stop the exercise session and see a doctor for a proper diagnosis.
__________________________________________________________________
 Amanda Vogel, M.A., holds a master’s degree in human kinetics and is a certified fitness professional in Vancouver, B.C. In addition to being an online marketing consultant for BOSU, Amanda owns Active Voice, a writing, editing and consulting service for the fitness industry. Her articles have appeared in Women’s Health, SELF and Prevention. You can reach her at www.ActiveVoice.ca, http://FitnessWriter.blogspot.com or www.twitter.com/amandavogel.
Amanda Vogel, M.A., holds a master’s degree in human kinetics and is a certified fitness professional in Vancouver, B.C. In addition to being an online marketing consultant for BOSU, Amanda owns Active Voice, a writing, editing and consulting service for the fitness industry. Her articles have appeared in Women’s Health, SELF and Prevention. You can reach her at www.ActiveVoice.ca, http://FitnessWriter.blogspot.com or www.twitter.com/amandavogel.