
By CARL FOSTER, Ph.D., and JOHN P. PORCARI, Ph.D.
Department of Exercise and Sport Science, University of Wisconsin-La Crosse
“If you can just talk, you are just about at the right exercise intensity.” I first heard this simple concept from a fellow late-night runner at the Memorial Stadium track at the University of Texas at Austin. It was the summer of 1979, and I was a first-year graduate student in exercise physiology, still in wonder as I began to learn things like VO2max, lactate threshold, mitochondrial density and training effect. And yet here was some guy I barely knew telling me that I could design my training intensity based on being able to talk. Surely he was misguided and simply lacked the technological knowledge he needed to guide his training. But as it turned out, he was pretty much right.
Known But Not Necessarily Respected
Even in 1979, the concept of the “Talk Test” as a marker of correct exercise intensity was not really all that new. In fact, it has been around at least since 1939, when Professor John Grayson at Oxford University advised English mountaineers to “climb no faster than you can talk.” This simple idea kept kicking around on the fringes of exercise physiology, not quite technologically advanced enough to ever gain real respectability in an era of rapidly expanding technology, but never quite going away. It was included in the fourth edition of ACSM’s Guidelines for Exercise and Training in 1991, and in guidelines published by the American Council on Exercise in 1997. But despite official recognition by the major professional societies, the Talk Test never quite achieved the respectability of the Karvonen Method or the glamour of the newly emerging exercise-prescription techniques such as %VO2max, ventilatory threshold, or techniques based on analysis of blood lactate.
In the late 1990s, Dr. Robert Goode at the University of Toronto began promoting the “hear your breathing test,’ and Dr. Steven Keteyian and colleagues at Henry Ford Hospital in Detroit demonstrated that if people could still talk well enough to answer questions to a structured interview (e.g., What did you have for breakfast this morning?), they were in a range of heart rate or VO2 that fit the exercise prescription guidelines of ACSM.
Talk Test Talking Points
- Ongoing research confirms that the Talk Test is a valuable tool for monitoring (and controlling) exercise intensity.
- Studies in a variety of populations, including healthy individuals, cardiac patients, and athletes, have demonstrated that the Talk Test is a very good marker of VT1.
- At an intensity level above VT1, but below VT2, an exerciser will still be able to speak, but not comfortably.
- VT2 represents the point at which high-intensity exercise can no longer be sustained due to the accumulation of lactic acid.
- The Talk Test can be administered in a variety of ways, including reciting something familiar such as the Pledge of Allegiance, or reading from a text. After the recitation, if they can answer “yes” to the question, “Can you speak comfortably?”, then their intensity level is below VT1.
- If the client hesitates or answers equivocally to this question, their intensity is probably right at VT1.
- If the client answers no, they are probably close to or above VT2.
- Compared to %VO2max or %MHR, the Talk Test has several advantages as a method of programming and monitoring exercise because it is based off an individual’s unique metabolic or ventilatory responses.
- The Talk Test is a particularly good marker for those who want to lose weight because at VT1, fats continue to contribute significantly to the number of calories burned.
- Additionally, training at or near VT1 increases the likelihood of a better exercise experience and enhances long-term adherence.
Validating the Talk Test
It was about this time that I joined Dr. John Porcari at the University of Wisconsin, La Crosse. John and a graduate student named Meghan Dehart were talking about ways they could follow up on some of Keteyian’s work with a project on the Talk Test. First, we reasoned that the Talk Test must be close to the ventilatory threshold, since breathing frequency increases rapidly at the point of the ventilatory threshold, and the one thing you have to do to be able to talk comfortably is to control the frequency of your breathing. During practice trials in the laboratory, we figured out that the simplest way to do the Talk Test was to have the subject recite aloud a standard paragraph and then ask them if they can speak comfortably. For several exercise stages the response to our question would be a quick “Yep,” but sometime in the middle of the test the subject would begin to equivocate: “Yeah, but….” And still later in the test, when the subjects were working really hard, the answer to our question was a flat “No.”
Because you can’t talk and do gas exchange studies at the same time, we had our subjects do the same exercise tests on two different days. We found that as long as the subject was responding to our question about talking comfortably with “Yep,” that they were at an exercise intensity below the ventilatory threshold. We also observed that just at the point where the subject’s answers about speech comfort started to become equivocal, that they were right on top of the ventilatory threshold. We now had a way of doing the Talk Test that seemed to work, and had shown that it served as a surrogate for an important physiological marker—ventilatory threshold—that was otherwise only measureable in a high-tech laboratory setting. Feeling good about our results, we wrote up the research for publication and moved on to other investigations.
It turns out, however, that the story of the Talk Test—and our study of it—was just beginning. Each year brought a new crop of graduate students with new research ideas and ways of analyzing the Talk Test. While our previous study had used a standard paragraph out of the speech therapy literature (“The Rainbow Passage”), graduate student Natalie Schaffer showed that the “Pledge of Allegiance” worked just as well. Then Stacey Voelker demonstrated that the Talk Test was just as good of a marker of the ventilatory threshold in stable cardiac patients and athletes as is had been in the university students that Meghan and Natalie had used. Pedro Recalde next showed that the tail end of the Talk Test, the place where the subject says a flat “no” to the question “can you talk comfortably?” was a reasonable marker of another physiologic benchmark—the respiratory compensation threshold (VT2). About this same time, Amy Kelso found that it didn’t matter what strategy we used to provoke speech—a standard paragraph or the structured interview used at Henry Ford Hospital in Detroit—the results of the Talk Test were the same. And Rachel Persinger demonstrated that the Talk Test was equally good at identifying the ventilatory threshold on the treadmill or the cycle ergometer.
So, with the research efforts of six graduate students, it became clear that not only did the Talk Test provide an accurate but very simple marker of more complex physiologic processes, it might even help guide exercise prescription. These early results are summarized in Figure 1, which shows that below the ventilatory threshold, comfortable speech is usually possible (green zone); that right at the intensity of the ventilatory threshold comfortable speech becomes equivocal (yellow zone); and right at the respiratory compensation threshold, comfortable speech becomes impossible (red zone).
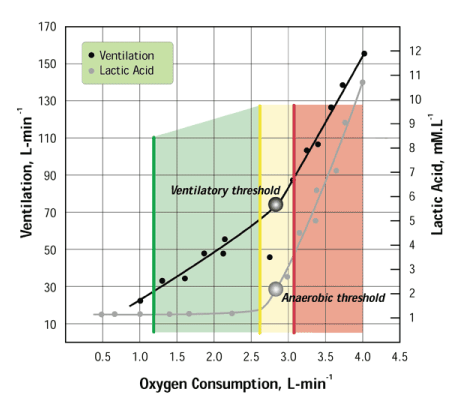
Figure 1 illustrates the relationship between ventilatory threshold, anaerobic threshold, and the ability to “talk.” The green zone represents the appropriate exercise-training zone where individuals have a “positive” talk test, indicating that they can still speak comfortably. The yellow zone corresponds to the point where speaking begins to become difficult—the “equivocal” stage of the talk test. Exercising at this intensity is difficult and cannot continue indefinitely. The red zone, which corresponds to the point where smooth conversation becomes impossible, is the “negative” stage of the Talk Test and exercising at this level rapidly results in fatigue.
Making Exercise Safer for Cardiac Patients
John and I are both grounded in clinical exercise physiology, and want to apply our skills to helping clients and patients exercise safely. In Germany, Dr. Katharina Meyer had shown that in patients with heart disease, the ventilatory threshold often occurred before the first ECG abnormalities that indicated that the heart muscle was getting ischemic (i.e., not getting enough blood flow). We reasoned that if this were true, and if the Talk Test was a basic marker of the ventilatory threshold, then patients should not be able to talk comfortably if they were having myocardial ischemia.
To test this theory, graduate student Christine Cannon administered the Talk Test during diagnostic stress tests at a local hospital. She selected 20 tests that the attending physician had diagnosed as consistent with exertional myocardial ischemia (e.g., a “positive’ exercise test). All of these patients had reached the equivocal stage of the Talk Test before the first appearance of electrocardiographic abnormalities, based on either workload or heart rate. In fact, the difference in heart rate from the last time they could speak comfortably and the first electrocardiographic abnormalities was about 10 beats per minute, the same margin that the ACSM Guidelines for Exercise Testing and Prescription recommends for prescribing exercise in patients with exertional ischemia. These were very exciting findings, because they suggested that if people could talk during exercise, then it was unlikely that they had exertional ischemia. Importantly, the biggest safety concern in clinical exercise programs could be addressed with a very simple technique.
Digging Deeper Into the Talk Test
Up to this point, we had taken an essentially correlative approach to studying the Talk Test during incremental exercise (e.g., exercise testing), comparing Talk Test responses to metabolic-exercise responses measured using respiratory gas exchange. It was time for a deeper look at the Talk Test and how it related to exercise responses during exercise training.
“If we’re going to keep talking, you’re going to have to slow down.” Recalling this statement from my college running days, we reasoned that if we varied the workload above and below the ventilatory threshold, that subjects would lose and gain the ability to speak comfortably. Denise Smaczny undertook this study and her findings were mostly what we expected, except that a certain number of people could still talk at the point when we expected them to no longer be able to. In a follow-up study, Holly Webber demonstrated that if the exercise intensity is only slightly above the ventilatory threshold, it takes two to four minutes to be able to lose the ability to speak. However, the basic relationship—below ventilatory threshold, speech is comfortable, and above ventilatory threshold, speech is not comfortable—remains valid.
Next, we investigated whether or not the relationship between the Talk Test and the ventilatory threshold was stable. First, Jennifer Anderson, using blood donation designed to reduce the ventilatory threshold, and later Melissa Paulson, using exercise training designed to increase the ventilatory threshold, demonstrated that the Talk Test was able to accurately track experimental modifications in the ventilatory threshold. In fact, they found that the changes in ventilatory threshold and the Talk Test responses were highly correlated: When the ventilatory threshold got better, then the workload eliciting the Talk Test got better.
Next, we wondered if the Talk Test responses during an incremental exercise test could be used to prescribe an appropriate exercise intensity for steady-state exercise. We knew from the results of Denise Smaczny and Holly Webber that there was a time lag between when the workload changed and Talk Test responses changed. Accordingly, our most recent study, conducted by Neepa Talati, involved performing incremental exercise tests on sedentary students. These same students then performed exercise training bouts at the work loads associated with the equivocal (+/-) stage, at the last positive stage, and at the stage prior to the last positive stage. She found that when the subjects exercised at the intensity associated with either the last positive or equivocal stages of the Talk Test, their responses during the training bout were unstable, and their levels of %HRmax, RPE, or speech comfort were greater than desirable. Thus, it appears that the stage prior to the last positive stage during incremental exercise is the highest exercise intensity that leads to appropriate exercise responses during exercise training, at least in sedentary individuals.
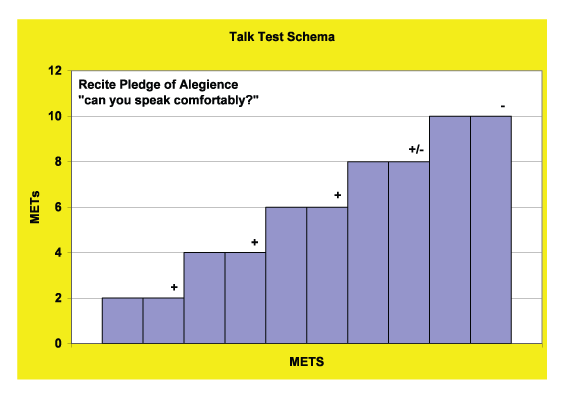
Figure 2 illustrates the practical application of the Talk Test. If you to use the Talk Test to guide a client’s exercise program, have him or her perform an incremental exercise test (e.g., on a treadmill, cycle ergometer, elliptical machine). Start at a low exercise workload and exercise for two minutes. Recite the Pledge of Allegiance. Every 2 minutes increase the workload by about 10 percent and recite the Pledge of Allegiance at the end of each stage. When you get to the last stage where the client can speak comfortably (i.e., without having to take breaths between every few words), he or she has reached the Last Positive Stage of the Talk Test. Drop back one stage (workload) below that point. This is the exercise workload that the client should be able to maintain for a 30- to 45-minute workout.
Conclusion
Thus, as unlikely as it might seem, we’ve known for decades how to prescribe exercise using the Talk Test. We just didn’t have the data to show that Professor Grayson’s recommendation to British mountaineers, more than 70 years ago, was indeed very good advice. Not only does the Talk Test provide a very useful tool for establishing and monitoring exercise intensity, but it may also contribute to the safety of exercise training.
For more information about VT1, VT2 (respiratory compensation threshold) and the ability to talk in each of these three training zones, click the image above to view a video demonstration.
____________________________________________________________________________
 Carl Foster, Ph.D., is a professor in the Department of Exercise and Sports Science and director of the Human Performance Laboratory at the University of Wisconsin–La Crosse (UWL). He is a fellow of the American College of Sports Medicine (ACSM) and of the American Association of Cardiovascular and Pulmonary Rehabilitation. He was the 2005–2006 President of ACSM. Dr. Foster’s research interests range from high-performance physiology (he is the head of sports science for U.S. Speedskating) to clinical exercise physiology (he is the research director for the Clinical Exercise Physiology graduate program at UWL). He has published more than 250 scientific papers and book chapters and 22 longer works (e.g., books, monographs, position stands, videos).
Carl Foster, Ph.D., is a professor in the Department of Exercise and Sports Science and director of the Human Performance Laboratory at the University of Wisconsin–La Crosse (UWL). He is a fellow of the American College of Sports Medicine (ACSM) and of the American Association of Cardiovascular and Pulmonary Rehabilitation. He was the 2005–2006 President of ACSM. Dr. Foster’s research interests range from high-performance physiology (he is the head of sports science for U.S. Speedskating) to clinical exercise physiology (he is the research director for the Clinical Exercise Physiology graduate program at UWL). He has published more than 250 scientific papers and book chapters and 22 longer works (e.g., books, monographs, position stands, videos).

John P. Porcari, Ph.D., is a professor in the Department of Exercise and Sports Science and executive director of the La Crosse Exercise and Health Program at the University of Wisconsin–La Crosse. He is a fellow of the American College of Sports Medicine and of the American Association of Cardiovascular and Pulmonary Rehabilitation (AACVPR) and was the President of AACVPR in 2002–2003. Dr. Porcari’s research interests have focused on the acute and training responses to exercising on a variety of exercise modalities, particularly new fitness products. He has authored more than 75 peer-reviewed publications and made more than 150 national presentations dealing with health and fitness.